Experimental test by replacing fine bran with coarse bran in einkorn wheat flour
The results obtained in the present work suggest that the particle size of the fibrous fraction may represent a relevant technological parameter in the design of doughs with a weak gluten network or limited structural development capacity, as in the case of whole einkorn.
The experimental observation could also be of interest for other bread systems characterized by visco-plastic doughs, including some gluten-free systems, in which the structure of the dough depends to a greater extent on the interactions between the liquid phase and dispersed solid particles.
Analysis of results – Test no. 3 of 10-04-2026
Introduction
The present work continues a series of experimental trials dedicated to breadmaking with whole einkorn wheat flour (Triticum monococcum), a raw material that shows technological characteristics different from those of modern soft wheats and a limited gluten development capacity. Previous test (09-03-2026): Experimental application of an advanced method for the production of bread doughs with flours of limited gluten development capacity.
This characteristic is linked to the particular protein composition of einkorn, which generally presents a lower quantity of high-molecular-weight glutenin polymers and a different distribution of gliadins. Gliadins mainly contribute to the viscosity and extensibility of the dough, whereas glutenins are responsible for the formation of an elastic network capable of effectively retaining fermentation gases.
A relatively high gliadin-to-glutenin ratio therefore tends to produce doughs that are less elastic and more viscous than those obtained from modern soft wheat [Shewry & Halford, 2002; Wieser, 2007].
This technological condition is often also reflected in the empirical perception of the dough, which may appear visco-plastic, sticky and difficult to handle, with a consistency that during manual processing is sometimes described as similar to “modeling clay” (“pongo”).
In the previous test of 09-03-2026 a 600 µm sieving was adopted, with redistribution of the fractions in the biga and in the final dough.
In the current test of 10-04-2026 a significant modification was introduced in the preparation of the raw material: the flour was sieved at 500 µm and the removed bran was replaced with an equal weight of coarser bran, with particle size between 800 and 600 µm, thus reconstructing a reorganized whole flour.
The experimental hypothesis was to verify whether an einkorn dough containing a coarser bran fraction could show, compared with the previous test:
1. better dough workability
2. greater stability during proofing
3. a more open crumb structure.
Synthetic comparison between the first and the second test
|
Parameter |
Test 09-03-2026 |
Test 10-04-2026 |
|
Initial flour |
1800 g |
1800 g |
|
Sieve |
600 µm |
500 µm |
|
Separated bran |
85 g |
146 g |
|
Passing flour |
1715 g |
1654 g |
|
Bran reintroduction |
original bran |
bran with coarser particle size (coarse bran) 800-600 µm |
|
Final dough |
1000 g |
1000 g |
|
Pre-dough (biga) |
800 g |
800 g |
Materials and flour reorganization
The raw material used in the test of 10-04-2026 consists of stone-milled whole einkorn wheat flour for a total quantity of 1800 g.
The flour was entirely sieved with a 500 µm mesh, obtaining:
- 146 g of bran fraction
- 1654 g of passing flour
The separated bran fraction was subsequently replaced with an equal weight of coarser bran, with particle size between 800 and 600 µm, thus reconstructing 1800 g of reorganized whole flour.
The distribution of the flour in the different stages of the process was as follows:
- Final dough: 1000 g of reorganized whole flour
- Pre-dough (biga): 800 g of reorganized whole flour
Post-maturation operational sequence
In the previous test of 09-03-2026, after 24 hours of maturation at about 5 °C, the dough was taken out of the refrigerator and subjected to progressive warming on a warm surface at about 20 °C, covered with a silicone mat lightly greased with olive oil, with a sequence of folds and resting periods.
In that test it was observed that heat penetrated the dough mass with difficulty: after about two hours only a small part of the bottom was warmed, while the upper layers still remained cold.
This heating difficulty can also be interpreted from a physical point of view. High-hydration doughs with visco-plastic behavior indeed have low thermal diffusivity, that is, a limited capacity to transmit heat from the outside toward the inside of the mass.
In bread doughs heat transfer occurs mainly by conduction and the speed with which temperature is distributed depends on the structure of the system and on the water content. In very viscous systems molecular mobility is reduced and heat diffusion is slower than in more fluid or more porous systems [Singh & Heldman, 2014].
In the specific case of whole einkorn doughs, the combination of:
- high dough viscosity
- relatively weak protein structure
- presence of the bran fraction
may contribute to slowing down heat diffusion within the mass.
In the present test some operational modifications were therefore introduced to improve thermal distribution:
- warm surface brought to about 24 °C
- dough slightly flattened after removal from refrigeration
- turning of the dough every 30 minutes for about 2 hours
These modifications aim to increase the thermal exchange surface and reduce the effective thickness of the mass, promoting a more uniform distribution of temperature inside the dough.
It also emerged that at this stage it is advisable to keep the room temperature not higher than 20-21 °C, in order to avoid the premature appearance of surface ruptures.
Experimental results
Dough after cold maturation
After 24 hours at about 5 °C, the surface of the dough appears uniform, smooth and continuous, without evident signs of collapse (Photo 1).

When the dough is turned out onto the warm surface, the bottom shows a continuous structure with localized openings, due to the expansion that occurred during the transfer from the bowl to the work surface (Photo 2).
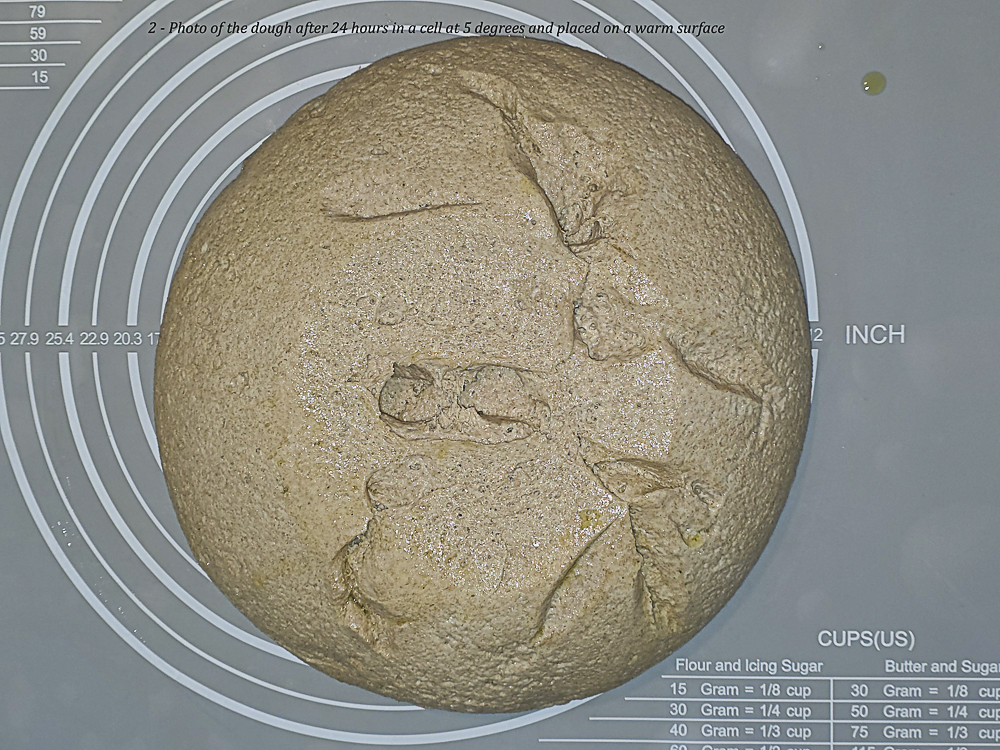
This stage does not suggest structural collapse, but rather a condition of dough relaxation. The cold slows down fermentative and biochemical processes but does not stop them completely; the dough therefore appears as a biochemically modified but mechanically relaxed system.
Prolonged dough maturation is known to progressively modify the protein structure and the enzymatic activity of the flour, improving dough extensibility and influencing the final structure of the bread [Gobbetti et al., 2014].
Critical phase after removal from refrigeration
During its stay on the warm surface, the dough goes through a phase in which the network is temporarily fragile.
The photograph immediately preceding manipulation is missing, but at that moment the dough showed moderate surface ruptures.
The available images show that, after manipulation and subsequent resting, the surface tends to compact again and become homogeneous (Photo 3). Even after about three hours in total on the warm surface, at the moment of transfer to the proofing basket, the surface once again appears continuous and regular (Photo 4).


The observed sequence can be summarized as follows:
1. removal from refrigeration with a fragile network
2. appearance of moderate surface ruptures
3. manipulation of the dough
4. resting on the warm surface
5. recompaction and reorganization of the surface
This behavior suggests that the protein network, although temporarily weakened, retains a capacity for reorganization.
The restructuring of the protein network observed is consistent with the model of formation and reorganization of the Glutenin MacroPolymer described by Wieser [Wieser, 2007].
Observations on dough workability
During manual processing, the dough containing the coarser bran appears decidedly more workable than that observed in the previous test.
To the hands the dough is:
- less sticky
- less viscous
- less pasty
During manual manipulation the dough shows a plastic and weakly elastic consistency, with relatively stable deformation under the action of the hands and a limited capacity for elastic recovery.
From a biochemical point of view, this behavior is consistent with the protein composition of einkorn. The greater relative incidence of gliadins compared with glutenins indeed tends to produce doughs with predominantly plastic behavior and limited elasticity, in which deformation occurs more by viscous flow than by elastic recovery [Shewry & Halford, 2002].
The tactile perception is that of a more manageable and less adhesive mass, with an internal structure that is easier to interpret during manual processing [Dobraszczyk & Morgenstern, 2003].
Manual evaluation of the dough represents an important element in the rheological assessment of complex flour systems. Alongside instrumental tools such as the alveograph and farinograph, the baker’s manual experience makes it possible to interpret characteristics such as adhesiveness, elasticity and extensibility of the dough [Dobraszczyk & Morgenstern, 2003].
The greater workability observed in the present test can plausibly be linked to the coarser particle size of the bran fraction, which interferes less with the liquid phase of the dough and with the continuity of the protein network.
Final proofing
The dough is placed in the proofing basket only when it already appears sufficiently developed on the warm surface.
In these doughs it is in fact preferable to push proofing on the warm surface rather than in the basket, since they tend to develop more easily laterally than vertically.
The photograph of the dough at the end of proofing is particularly significant (Photo 5).

The surface shows diffuse ruptures, but the structure nevertheless continues to expand. From the moment in which the surface was still intact until the moment of the end of proofing, the dough continued to expand, rising by about 1 cm.
Despite the surface fractures, the shape of the dough remains substantially spherical, without flattening or evident lateral collapse.
This behavior suggests that the ruptures mainly affect the superficial layer of the dough, while the internal structure still maintains sufficient capacity to retain fermentation gases.
Baking, crust and final development
Baking was carried out with the same protocol as the reference test.
The bread shows orderly development, with a readable opening and well-directed growth (Photo 6).

The multiple fracture observed during baking is an intentional consequence of the method of placing the dough in the container: the dough is formed by closing the flaps without sealing them completely, subjected to slight rounding, and then placed upside down in the baking container, so that the heat naturally opens the unsealed flaps.
Crumb
The section of the bread shows a fine-medium internal structure, with alveoli distributed relatively uniformly and with some irregularities also attributable to the air incorporated during handling.
The lower part of the slice does not show a compact layer but presents alveoli also in the lower area, generally critical in weak or whole doughs (Photo 7).

Observation of the slices confirms an elastic crumb, slightly moist but not sticky, free of anomalous cavities or massively compact areas (Photos 8 and 9).


The photograph of the base of the bread shows complete baking, with superficial microfractures and the absence of compressed or collapsed areas (Photo 10).

The comparison between the bread from the first baking and that from the second baking, shaped more freely as a “ciabatta”, shows a comparable internal structure, albeit with a different expansion geometry (Photo 11).

The comparison between the section of the bread from the first test (Photo 20 but above all Photo 21) and that of the


second test (Photo 8) shows an alveolar structure that is partly different. In both cases the crumb structure is characterized by small-medium alveoli, typical of whole einkorn doughs; in the second test, however, there is a lower presence of areas with more compact crumb, particularly visible in the left area of the slice from the first test, and a greater participation of the lower part of the crumb in alveolar development.
This suggests that the particle size of the bran fraction may influence not only the viscosity of the dough and its deformability during proofing, but also the distribution of fermentative thrust within the dough mass.
In the second test, the presence of bran with a coarser particle size (coarse bran) seems to be associated with a more uniform distribution of alveoli in the crumb and with a more extensive involvement of the base of the bread in the development of the alveolar structure.
Overall, the observation suggests that a coarser bran fraction may contribute to reducing the formation of locally more compact zones in the crumb, while maintaining an overall fine but more homogeneous texture. This behavior is consistent with the hypothesis that bran particle size acts mainly on dough viscosity, on the deformability of the structure and on the mode of expansion during proofing, indirectly also influencing the distribution of alveoli in the crumb.
The comparison between the two sections also suggests a different distribution of fermentative thrust within the dough. In the second test the presence of bran with a coarser particle size seems to be associated with a more extensive participation of the lower part of the crumb in alveolar development, indicating a more uniform distribution of gas pressure in the dough mass. (I Test photos )
Physical interpretation of dough behavior
The experimental results observed in the present work can be interpreted in light of the particular protein structure of einkorn and of the interaction between the protein matrix, water and the fibrous fraction of whole flour.
Unlike modern soft wheats, einkorn generally contains a lower quantity of high-molecular-weight glutenin polymers and a different distribution of gliadins.
Gliadins mainly contribute to dough viscosity and extensibility, whereas glutenins are responsible for the formation of an elastic network capable of retaining fermentation gases.
A relatively high gliadin-to-glutenin ratio therefore tends to produce doughs that are less elastic and more viscous, with rheological behavior that can be defined as visco-plastic [Shewry & Halford, 2002; Wieser, 2007].
This characteristic is consistent with the empirical perception of the dough described during the experiment, in which the mass shows a visco-plastic consistency that during manual processing is sometimes perceived as a compact and moldable mass, similar to “pongo”.
Effect of bran particle size
One of the central aspects of the present work concerns the influence of the particle size of the bran fraction on dough behavior.
The scientific literature clearly shows that the size of bran particles significantly influences the rheological properties of whole doughs.
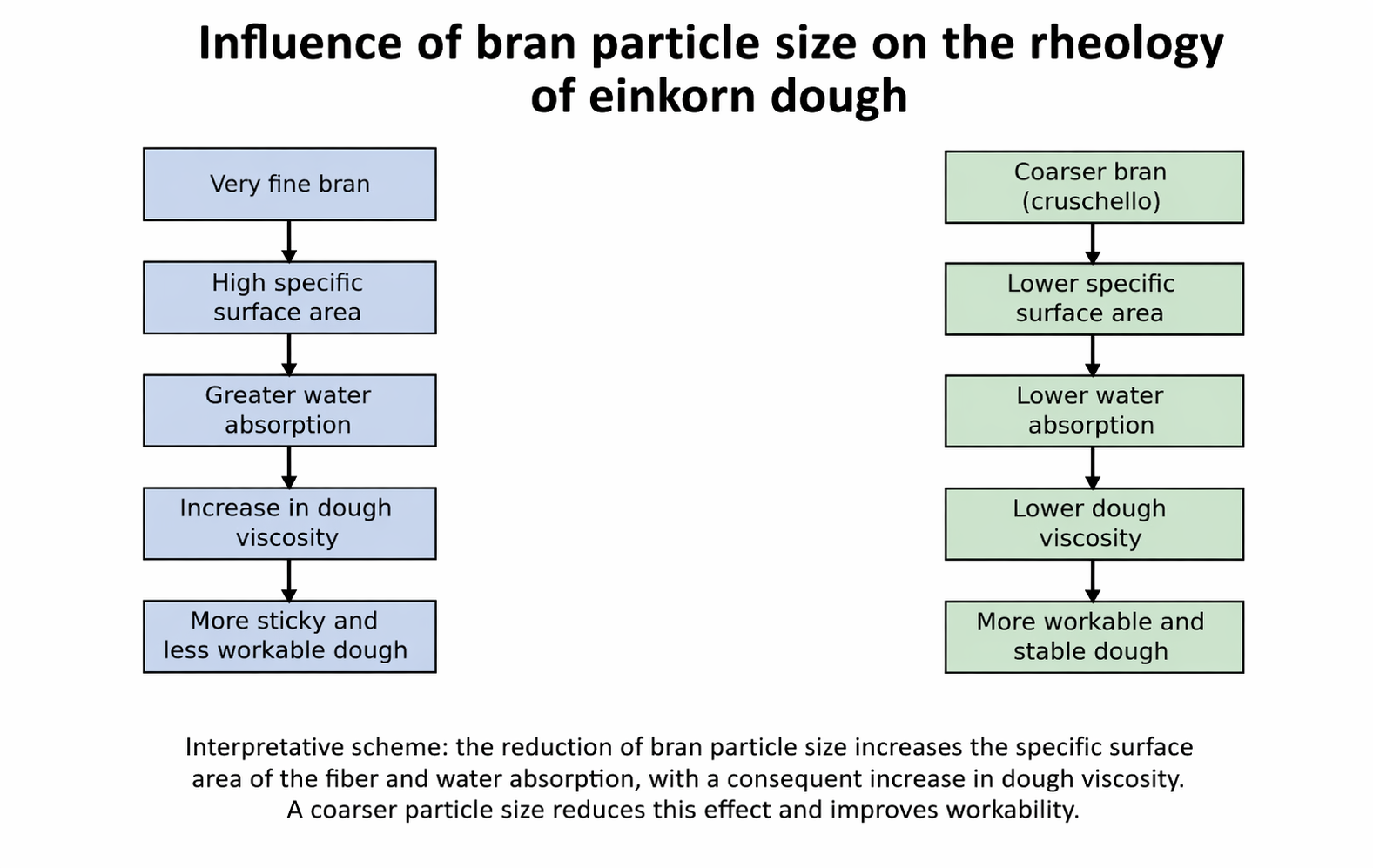
Very fine bran particles have a high specific surface area and tend to:
- increase water absorption
- increase dough viscosity
- interfere with the continuity of the gluten network.
Coarser particles, on the contrary, interfere less with the protein structure and allow better bread expansion.
This behavior was demonstrated experimentally in the study by Noort and co-workers, which analyzed the effect of bran particle size on bread quality [Noort et al., 2010].
A similar result emerges from the systematic review by Cappelli and co-workers, which highlights how the reduction of whole flour particle size tends to increase dough viscosity and worsen its workability [Cappelli et al., 2019].
Bran and gluten structure
The role of bran in breadmaking had already been studied in the 1970s.
One of the classic works is that of Pomeranz and co-workers, who showed how the fiber present in bran can:
- interrupt the continuity of the gluten network
- absorb water
- modify the rheological properties of the dough.
The effect of bran on the protein network depends significantly on the size of the particles [Pomeranz et al., 1977].
Very fine particles indeed tend to interfere more with the continuity of the protein network, whereas larger particles exert a less marked effect.
Interpretation of the behavior observed in the test
The experimental observations made during the test suggest that the coarser particle size of the bran may directly influence the overall viscosity of einkorn dough.
In einkorn the dough is already predisposed to viscous behavior because of its protein composition.
When the bran is very fine:
1. the contact surface with water increases
2. water absorption increases
3. the amount of free water in the system decreases
4. dough viscosity increases.
This phenomenon can amplify the viscous effect due to gliadins.
When, on the other hand, the bran is coarser:
- the contact surface is smaller
- a greater share of water remains in the continuous phase of the dough
- the overall viscosity of the system decreases.
The result is a dough perceived as less sticky and easier to handle.
This interpretation is consistent with the manual observations made during the experiment, in which the dough containing bran with a coarser particle size (coarse bran) was easier to manage by hand and more stable during proofing.
Reorganization of the protein network
Another interesting element that emerged during the experiment concerns the capacity of the dough to recompact after the appearance of surface ruptures.
During the warming phase on the warm surface the dough showed moments in which the network appeared fragile and discontinuous, followed by subsequent recomposition of the surface.
This behavior suggests that the protein network may pass through temporary phases of discontinuity without completely losing the capacity to reorganize itself.
The restructuring of the protein network observed is consistent with the model of formation and reorganization of the Glutenin MacroPolymer described by Wieser [Wieser, 2007].
Manual evaluation of dough rheology
The tactile perception of the dough during processing represents an important element in the evaluation of the rheological properties of complex flour systems.
Alongside instrumental tools such as the alveograph and farinograph, manual evaluation by the baker makes it possible to interpret characteristics such as:
- adhesiveness
- elasticity
- extensibility
- resistance to deformation.
This aspect was highlighted in the study by Dobraszczyk and Morgenstern on the relationship between dough rheology and the breadmaking process [Dobraszczyk & Morgenstern, 2003].
In complex systems, such as whole doughs or high-hydration doughs, tactile perception can provide information that standard rheological instruments are not always able to capture.
Comparative summary table of the two tests
|
Parameter |
Test 09-03-2026 |
Test 10-04-2026 |
|
Sieving |
600 µm |
500 µm |
|
Reintroduced bran |
original bran |
bran with coarser particle size (coarse bran) 800-600 µm |
|
Dough workability |
stickier, more viscous |
more workable |
|
Behavior during proofing |
more vertical development |
greater lateral expansion |
|
Dough stability |
good |
very good |
|
Bread height |
7-7.5 cm |
5.5 cm |
|
Dough weight |
~780 g |
1762 g |
|
Weight loss |
16-17 % |
~22 % |
|
Crumb structure |
fine |
fine-medium |
Final interpretative synthesis
The set of visual observations, quantitative measurements and manual evaluations of the dough suggests that the particle size of the bran fraction may significantly influence the rheology of einkorn dough and proofing behavior.
In particular, the presence of bran with a coarser particle size appears to be associated with:
- lower dough viscosity
- better manual workability
- greater stability during proofing
- maintenance of the bread expansion capacity.
This behavior appears to be consistent with the scientific literature on bran particle size and the rheology of whole doughs [Noort et al., 2010; Cappelli et al., 2019].
Research perspectives
The results obtained in the present study indicate that the particle size of the fibrous fraction can represent a relevant technological parameter in the rheological behavior of doughs obtained from flours with limited gluten development capacity, as in the case of whole einkorn wheat.
The experimental observation according to which the use of a bran fraction with a coarser particle size is associated with a reduction in dough viscosity and with better manual workability suggests that the size of the solid particles dispersed in the system may significantly influence not only the viscosity of the system, but also the stability of the dough structure during proofing.
These results highlight the opportunity for further systematic studies on the relationship between the particle size of fibrous fractions and dough behavior, particularly in bread systems characterized by weak or only partially developed protein structures.
From this perspective, the possibility of modulating the particle size of the fibrous fraction – through the use of selected bran or other plant fibers with controlled dimensions – could represent a technological tool for regulating the rheological properties of doughs, with possible applications not only in breadmaking with ancient grains, but also in other complex bread systems, including some gluten-free doughs, in which the structure of the system depends to a greater extent on the interactions between the continuous phase and dispersed solid particles.
Overall, the results obtained suggest that the particle size of the fibrous fraction deserves greater attention as a technological variable in dough design, opening the way to further experimental studies on the role of insoluble particles in the structural dynamics of bread doughs.
Reference scientific studies
1. Effect of bran particle size on bread quality
Noort M.W.J., van Haaster D., Hemery Y., Schols H., Hamer R. (2010)
The effect of particle size of wheat bran fractions on bread quality
Journal of Cereal Science
DOI: 10.1016/j.jcs.2010.04.008
Brief abstract
The study analyzes the influence of bran particle size on the rheological properties of the dough and on bread quality. The authors separate bran into different particle-size fractions and observe that finer bran significantly increases water absorption and dough viscosity, reducing bread volume. Coarser particles interfere less with the gluten network and allow a more regular development of the bread structure.
These results are consistent with the experimental observations of the present work, in which the use of bran with a coarser particle size is associated with greater dough workability and better stability during proofing.
2. Particle size of whole wheat flour and bread quality
Cappelli A., Oliva N., Cini E. (2019)
A systematic review of the influence of whole wheat flour particle size on bread characteristics
Journal of Cereal Science
DOI: 10.1016/j.jcs.2019.102790
Brief abstract
This systematic review analyzes numerous studies on the influence of the particle size of whole flour and bran on dough properties and bread quality. The authors highlight that reducing particle size increases the specific surface area of the fiber and the water absorption capacity, resulting in increased dough viscosity and greater interference with gluten network formation. Whole flours with coarser particles instead show better workability and less interference with the protein structure.
3. Structure and function of gluten proteins
Shewry P.R., Halford N.G. (2002)
Cereal seed storage proteins: structures, properties and role in grain utilization
Biochemical Society Transactions
DOI: 10.1042/BST0300118
Brief abstract
The work analyzes the structure and function of the main cereal storage proteins, with particular attention to the role of gliadins and glutenins in the formation of the gluten network. Gliadins mainly contribute to the viscosity and extensibility of the dough, whereas glutenins are responsible for the formation of an elastic network capable of retaining fermentation gases. A high gliadin-to-glutenin ratio produces doughs that are less elastic and more viscous, a characteristic that is frequently observed in doughs obtained from einkorn.
4. Fermentation and dough maturation
Gobbetti M., De Angelis M., Di Cagno R. (2014)
Sourdough fermentation and wheat bread quality
Trends in Food Science & Technology
DOI: 10.1016/j.tifs.2014.02.012
Brief abstract
This work analyzes the role of prolonged fermentation in the biochemical modification of wheat doughs. The authors show that dough maturation involves progressive modifications of proteins and of the enzymatic activity of the flour, with effects on dough structure, its extensibility and the final quality of the bread. Prolonged fermentation may also favor the temporary relaxation of the protein network before its reorganization during processing.
Bibliography
Shewry P.R., Halford N.G. (2002)
Cereal seed storage proteins: structures, properties and role in grain utilization
Biochemical Society Transactions
DOI: 10.1042/BST0300118
Wieser H. (2007)
Chemistry of gluten proteins
Food Microbiology
DOI: 10.1016/j.fm.2006.07.004
Noort M.W.J., van Haaster D., Hemery Y., Schols H., Hamer R. (2010)
The effect of particle size of wheat bran fractions on bread quality
Journal of Cereal Science
DOI: 10.1016/j.jcs.2010.04.008
Cappelli A., Oliva N., Cini E. (2019)
A systematic review of the influence of whole wheat flour particle size on bread characteristics
Journal of Cereal Science
DOI: 10.1016/j.jcs.2019.102790
Gobbetti M., De Angelis M., Di Cagno R. (2014)
Sourdough fermentation and wheat bread quality
Trends in Food Science & Technology
DOI: 10.1016/j.tifs.2014.02.012
Dobraszczyk B.J., Morgenstern M.P. (2003)
Rheology and the breadmaking process
Journal of Cereal Science
DOI: 10.1016/S0733-5210(03)00059-6
Pomeranz Y., Shogren M.D., Finney K.F., Bechtel D.B. (1977)
Fiber in breadmaking – effects on gluten structure
Cereal Chemistry
Brandolini A., Hidalgo A. (2011)
Nutritional value of einkorn wheat
Journal of the Science of Food and Agriculture
DOI: 10.1002/jsfa.4462
